Electrolytes for Fasting: The Role of Electrolytes and My Personal Protocol
Most people don’t fail fasting because of hunger. They fail because of electrolytes. Headaches, dizziness, low energy, poor sleep - people assume it’s part of fasting. In most cases, it’s not - it’s an electrolyte problem.
⚡ Why Electrolytes Matter During Fasting
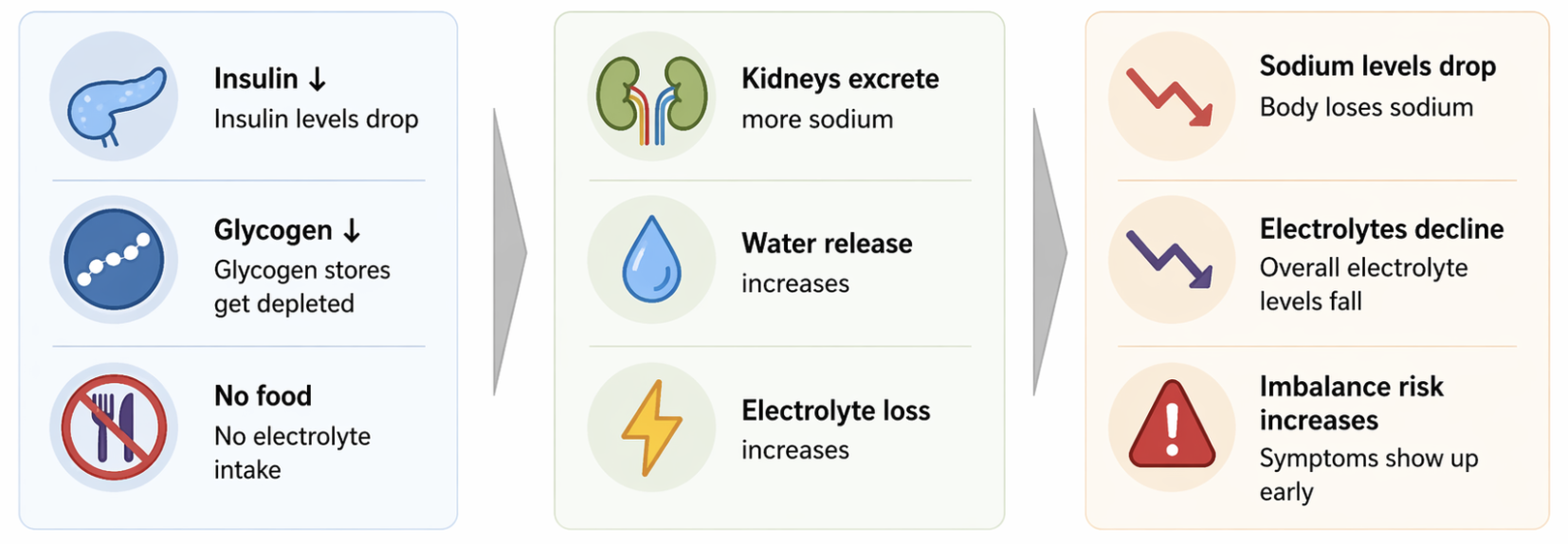
Fasting triggers a chain reaction in your body that leads to increased electrolyte loss. This visual shows how those changes happen step by step and why imbalance develops early.
This is the core reason why electrolytes for fasting are different from normal nutrition - and why many fasting symptoms are actually driven by electrolyte imbalance, not lack of food.
Now, if you don’t supplement electrolytes, it’s not immediately dangerous for most healthy people. The body will adapt and try to maintain balance by:
reducing sodium excretion through hormonal regulation
shifting fluids between compartments to maintain blood volume
lowering overall fluid volume across the body
increasing heart rate to compensate for lower blood pressure
But this compensation comes at a cost. You’ll likely feel dizziness, especially when standing, fatigue and low energy, headaches, brain fog and reduced physical and mental performance. So while fasting without electrolytes is possible, it’s often much harder than it needs to be.
Supplementing electrolytes doesn’t “make fasting work” - your body can do that. But it makes fasting significantly more stable, predictable, and tolerable.
🧂 The Only Electrolytes That Actually Matter
If you’re looking for a simple framework for fasting electrolytes, focus on three - sodium, potassium, and magnesium. For context, here are typical electrolyte levels in the blood
Sodium: 135–145 mmol/L
Potassium: 3.5–5.0 mmol/L
Calcium: 8.5–10.5 mg/dL
Magnesium: 1.7–2.2 mg/dL
Chloride: 98–106 mmol/L
Phosphate: 2.5–4.5 mg/dL
These levels are tightly regulated because they are critical for survival. During fasting, the body prioritizes keeping blood levels stable through kidney regulation, hormonal control, and fluid shifts. That’s why most electrolytes don’t require active management during a typical 7-10 day fast. Calcium is regulated by hormones, chloride follows sodium, phosphate becomes relevant mainly in very long fasts or refeeding, and trace minerals have large body reserves. In practice, everything comes down to three - sodium, potassium and magnesium.
These three electrolytes play distinct roles in how your body functions during a fast.
🎯 Exact Daily Targets During Extended Fasting
Sodium:
3,000-5,000 mg per day
4,000-6,000 mg if using sauna or steam room
up to 7,000 mg on heavy sweat days
Potassium: 1,000-2,000 mg per day
Magnesium: 300-400 mg per day
These are fasting-specific targets - not general nutrition guidelines.
⚖️ How This Differs From Non-Fasting Daily Requirements
Electrolyte needs during fasting are fundamentally different from normal nutrition.
Sodium: 1,500-2,300 mg on non-fasting days vs 3,000-5,000+ mg during fasting. Again, this difference is due to lower insulin levels during fasting, which cause the kidneys to excrete more sodium, along with additional losses from glycogen depletion and water release.
Potassium: 3,500-4,700 mg on non-fasting days vs 1,000-2,000 mg during fasting. Though potassium intake drops to zero without food, but the body increases conservation, reducing overall requirements during fasting.
Magnesium: 300-420 mg on non-fasting days vs 300-400 mg during fasting. This is because magnesium losses and requirements remain relatively stable, so needs don’t change much between fed and fasting states.
Key takeaway: what works when you’re eating does not work when you’re fasting.
💧 Electrolyte Mix Comparison
I rank electrolyte mixes based on four things: how well they cover potassium and magnesium, how much sodium they include, whether they add calories, and whether they include unnecessary ingredients or additives.
Potassium and magnesium carry more weight in this ranking because they are harder to get during fasting. Sodium is still important, but it’s easy to adjust separately with salt. I also rank zero-calorie and cleaner products higher, since they align better with fasting.
Comparison table of electrolyte mixes with key minerals, ingredients, and overall ranking.
This table removes sodium to focus on potassium and magnesium. Since sodium is easy to adjust separately with salt, this view highlights how well each mix covers the electrolytes that are typically harder to manage during fasting.
Comparison of electrolyte mixes without sodium, focusing on potassium, magnesium, calories, ingredients, and overall ranking.
🧪 My Electrolyte Strategy
For sodium, I keep it simple and use Himalayan salt, targeting around 4,000-6,000 mg per day.
Salt is your primary electrolyte source during fasting
For potassium and magnesium, I use an electrolyte mix - typically 3 packets of Ultima per day.
Ultima electrolyte drink mix
This setup works well overall: sodium is on target and magnesium is in a good range. Potassium ends up slightly underdosed, but I intentionally keep it on the more conservative side. Unlike sodium, potassium has a narrower safety range and directly affects heart rhythm, so I prefer to stay cautious rather than push higher doses.
🩸 What My Bloodwork Shows
Across multiple extended fasts, my blood electrolytes stayed stable:
Magnesium: 2.0-2.2 mg/dL
Potassium: 4.3-4.8 mmol/L
Sodium: 137-140 mmol/L
Even during 7-10 day fasts. At first glance, this suggests everything is fine, but it’s not. Your body tightly regulates blood electrolytes. When levels drop, it compensates by shifting electrolytes from cells into the bloodstream. So your labs can look normal while you still feel terrible.
Sodium, potassium and magnesium stay stable in blood - even during extended fasting
For more results and detailed data from my extended fasts, visit the Results page
📝 A Couple Practical Considerations
First, most electrolyte drinks don’t work well for fasting. They’re designed for workouts and usually don’t have nearly enough sodium.
Second, if you’re taking potassium and magnesium separately, it helps to take potassium earlier in the day and magnesium in the evening - that can make a noticeable difference for sleep.
Another point to watch is calories. Some electrolyte mixes have 20-50 calories per serving, which can break a fast.
Finally, while mineral water is fine to include, it’s not enough on its own - it contains some electrolytes, but nowhere near what you need during fasting.
⚠️ Can You Overdose Electrolytes?
Yes - especially potassium.
Sodium is generally safe as long as you stay hydrated. Going up to around 7,000 mg occasionally is fine, but consistently pushing that high is usually unnecessary.
Potassium is where you need to be more careful. It directly affects heart rhythm, so I prefer to stay within the 1,000-2,000 mg range.
Magnesium is pretty low risk overall, but if you go above roughly 500-600 mg, you’ll likely notice digestive issues.
In practice, the bigger problem isn’t overdose - it’s imbalance.
🔬 Why Scientific Recommendations Are Lower
You may see lower recommendations in scientific literature. These numbers are not wrong - they are based on different goals and conditions. Most studies focus on 12–24 hour fasting and intermittent protocols. At the same time, a more traditional approach, represented by physicians like Jason Fung, relies on the body’s ability to regulate electrolytes and recommends supplementing reactively based on symptoms. Extended fasts, however, create cumulative electrolyte loss and zero intake from food. So scientific recommendations are designed to ensure safety and prevent deficiency, not to optimize performance and eliminate symptoms.
My approach is different. Instead of reacting to symptoms, I use structured daily targets to prevent them in the first place. Both approaches can work, but a structured approach tends to be more predictable and easier to manage during extended fasts.
✅ Final Takeaway
Electrolytes play a key role during fasting. Getting them right won’t eliminate every challenge, but it can make your fast significantly easier and more tolerable. Sodium helps maintain fluid balance and energy levels. Potassium supports muscle function and overall stability. Magnesium helps with relaxation, sleep, and recovery.
If your fast feels harder than expected, it’s worth taking a closer look at your electrolyte intake before assuming it’s just part of the process.
🔗 Electrolyte Links
Redmond Re-Lyte - https://amzn.to/4e0LFjA
LMNT - https://amzn.to/4990mO7
Venture Pal - https://amzn.to/4sVdu0x
Ultima Replenisher - https://amzn.to/48lU2m7
Thorne - https://amzn.to/4d1JDyx
Nutricost - https://amzn.to/48Noeqs
Key Nutrients - https://amzn.to/4cu10YP
Nuun Sport - https://amzn.to/4e7D9iL
📚 References
Research on electrolytes during fasting is less popular than topics like autophagy, but the physiology is well understood and strongly supported. Here are some of the most relevant papers that back up the key mechanisms.
“Fuel Metabolism in Starvation” 🔗 – A classic review explaining how the body shifts fuel use during fasting, including hormonal changes that increase sodium excretion and alter electrolyte balance.
“Starvation in Man” 🔗 – Landmark study detailing metabolic and electrolyte adaptations during prolonged fasting in humans.
“The effect of insulin on renal sodium metabolism. A review with clinical implications” 🔗 – Demonstrates that insulin promotes sodium retention, which explains why sodium loss increases when insulin drops during fasting.
“Variation in Total Body Water with Muscle Glycogen Changes” 🔗 – Shows that glycogen depletion leads to significant water loss, supporting the link between glycogen breakdown and electrolyte loss.
“Glycogen Storage: Illusions of Easy Weight Loss, Excessive Weight Regain, and Distortions in Estimates of Body Composition” 🔗 - Supports the point that early weight loss is heavily driven by glycogen and water, not just fat.
“Hyponatremia” 🔗 – Explains sodium regulation and why serum sodium levels may appear normal despite underlying imbalance or total body depletion.